Hip pain can be caused by a variety of injuries and underlying degenerative conditions. If you have tried other pain medications and conservative treatments with little to no effect on alleviating your pain, then our doctors can prescribe hyaluronic acid injections for hip pain - a substance injected directly into the affected hip joint with the aim to alleviate your discomforts.
If you want to learn more about the benefits of hip injections, Melbourne residents can contact us directly to arrange a consultation and discuss their options with our orthopaedic surgeon.
What is hyaluronic acid?
Hip joints contain a gel-like substance called synovial fluid. One unique component of the synovial fluid is hyaluronic acid. Its function is to cushion and lubricate the joint to ensure smooth gliding during joint activity.
As we age, or as a result of direct trauma or degenerative disease, the hyaluronic acid component can break down, reducing the effectiveness of the function of the synovial fluid. This will in turn result in pain and limited movement.
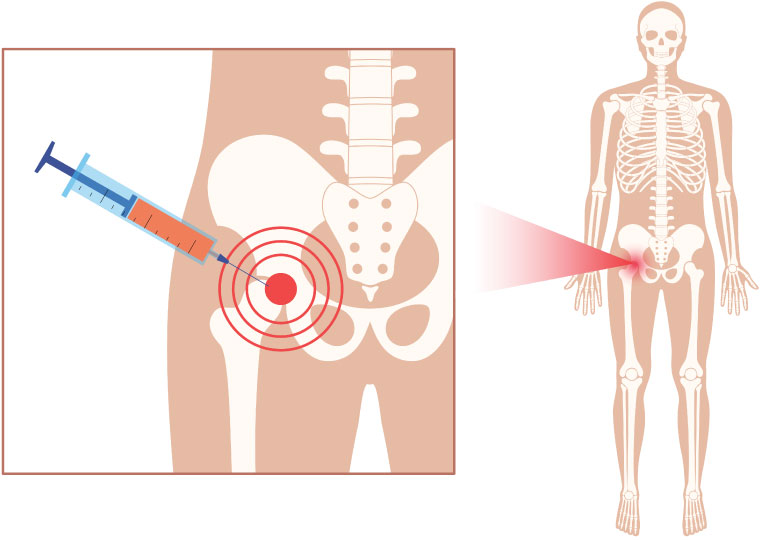
We inject the hyaluronic acid solution directly into the affected joint for maximum efficacy.
Thanks to advancements in medicine, scientists have formulated an injectable form of hyaluronic acid which has seen tremendous success in the treatment of osteoarthritis of the hip. Hip injections not only provide pain relief but also increase the viscosity of the synovial fluid, accentuating the ability of the joints to glide during movement, acting as a shock absorber to protect the soft tissue from trauma.
What are the benefits of hyaluronic acid injections for hip pain?
The use of hyaluronic acid in medicine has seen several benefits including:
- Management of joint pain - Studies show that injection of hyaluronic acid shows similar degrees of pain reduction as NSAIDs, without the unwanted gastrointestinal side effects.
- Anti-inflammatory - One study examining the effects of hyaluronic acid on the joints suggested that not only does it enhance the function of the synovial fluid, but also exerts some anti-inflammatory effects.
- Avoid surgery - This procedure has been seen to provide adequate pain alleviation to an extent that surgery may NOT be required or may be delayed. This, of course, will be determined upon consultation with your orthopaedic surgeon.
- Enhance your quality of life - Less pain means you can return to enjoying those fruitful moments of camaraderie amongst your family and friends. You will be able to enjoy more aspects of physical activity and enhance your quality of life.
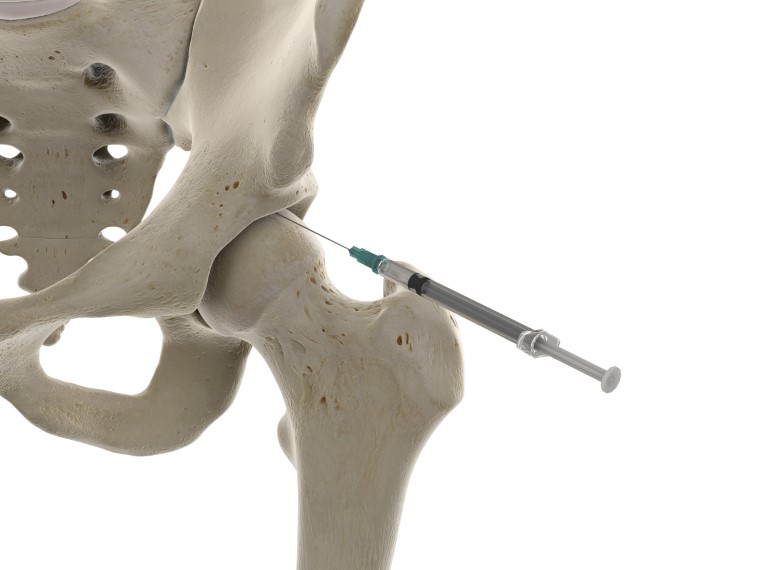
The injection will improve the function of the synovial fluid, leading to pain reduction and increased movements.
What hyaluronic acid injection therapy can cure?
Hip injections may be used to reduce pain and improve function in patients suffering from joint pain. The most common conditions treated by hyaluronic acid include:
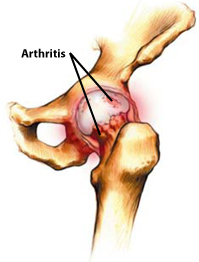
Arthritis damages the smooth lining of the joint called cartilage. This causes friction in the joint leading to pain and stiffness.
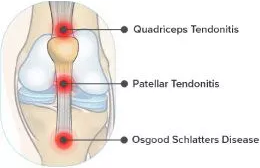
Tendonitis is inflammation of the tendon (attaches muscle to bone) which causes pain, swelling and loss of function.

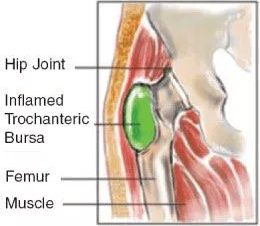
Bursitis is inflammation of the bursa (fluid-filled sacs between tendon and bone) which causes pain, swelling and loss of function.
Who is a good candidate for this procedure?
Those who have pain that is unresolved through traditional conservative treatments make good candidates for this procedure. This form of therapy is also beneficial for those who cannot, for any reason, receive cortisone injection treatments.
How is hyaluronic acid administered?
The injections are carried out in Dr Chandrasekaran’s rooms. The procedure takes 15 to 20 mins. The hyaluronic acid injection comes in a prefabricated syringe. For some, a local anaesthetic may be used to numb the area prior to treatment.
An ultrasound is used to guide the injection into the joint or tendon space. A dressing (the size of a bandaid) is used to cover the injection site which can then be removed the following day. Driving and normal activity can be resumed after the injection but strenuous activity should be avoided for 48 hours.
What are the unwanted side effects of this injection?
Injections are generally very safe. Most patients may experience mild pain upon administration of a single injection. However, as with all other non-surgical treatment options, following the injection of hyaluronic acid can cause the unwanted effects found below:
- A transient increase in pain that may last up to 72 hours
- Infection may develop 2-3 days following the injection and presents as fevers, chills, joint swelling, redness, reduced movement and inability to bear weight. If these symptoms develop it is important that you present for urgent medical review
- Tendon rupture may occur with repeated corticosteroid injections. For this reason repeat, cortisone injections are given at 4-month intervals
- Limited effect of the injection. In general, 70% of patients report a reduction in pain following injection. The effect of the injection is dependent on the severity of the disease, age and comorbidities. If one type of injection is not effective then another type is often trialed. There is no conclusive evidence of the superiority of one type of treatment over another
- There is no conclusive evidence that injections increase the subsequent risk of infection after surgery. However, there is usually a 6 week time lag between the injection and planned surgery
Our facility is equipped with state-of-the-art medical imaging to facilitate the effectiveness of our treatments.
How much does hyaluronic acid hip injections cost in Melbourne?
The total cost of your hyaluronic acid injection in Melbourne will vary depending on the number of injections you need, the site of treatment, and whether any additional complementary treatments are needed. A complete price breakdown of your procedure will be given to you during your initial consultation with Dr Chandrasekaran.
Why choose MOATI?
Our team at MOATI is dedicated to providing you with a premium level of care with the aim of getting you back on your feet to enjoy life’s precious moments. If you feel like our expertise could be of benefit to you, then give us a call to see just how we can help.

Dr Siva Chandrasekaran is a highly experienced Melbourne orthopaedic surgeon who specialises in both surgical and non-surgical treatments of hip and knee pain. He has honed his experiences from experts around the world having completed prestigious fellowships in the UK, USA and Switzerland.
FAQs
If you still have any unanswered questions regarding hyaluronic acid injections for the treatment of hip pain, then take a look at the section below.
Although these injections may come at a price, their investment value is priceless when taking into account their ability to resolve your pain issues and improve your mobility.
The length of hyaluronic acid treatments varies between individuals. For some, effects may last only weeks, whereas for others the results can be seen for several months.
Yes, you can walk after your injection.
NO