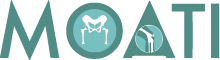
ACL injuries are amongst the most common sporting injuries reported in athletes. Studies suggest that ACL rupture accounts for 25-50% of all ligamentous injuries to the knee joint. The injury can often result in considerable pain alongside a significant reduction in movement and function of the joint.
Dr Siva Chandrasekaran has continued to develop his professional expertise to provide the ACL reconstruction patients can have in order to facilitate a rapid and complete return to normal daily activities.
What is Anterior Cruciate Ligament (ACL)?
The anterior cruciate ligament (ACL) is one of the four major ligaments that stabilize the knee joint. Its main function is to prevent the tibia (shin bone) from sliding forward and rotating on the femur (thigh bone). An intact ACL also assists with preventing excessive knee extension, knee varus, and tibial rotation. When intact, the ACL protects the meniscus from excess stress caused by athletic maneuvers or trauma.
Excessive force through direct trauma or stress can result in a rupture or tear of the ligament. A torn ACL can be life-changing if it occurs at an early age.
The ACL is one of 4 major stabilizing ligaments. When damaged, an individual will experience pain, swelling, and reduced mobility.
What is an ACL reconstruction?
ACL reconstruction surgery is a surgical or invasive procedure during which an orthopaedic surgeon will replace the torn ligament using grafts taken either directly from another part of your body o known as a donor site.
The surgery aims to provide pain relief, return mobility, and allow you to play sports involving running and other strenuous activities.
What are the causes of ACL tears?
An ACL injury is typically caused by twisting or hyperextension injuries. Sports activities like pivoting or sudden deceleration when running and falls during skiing are considered non-contact causes of ACL tears. Direct trauma to the back or side of the knee during collision sports is considered a contact injury to the ACL.
What are the symptoms of injury to the ACL?
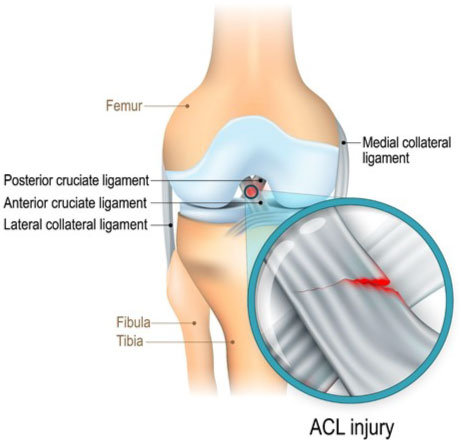
ACL tears cause immediate pain and are often followed by swelling, redness, and lack of mobility of the knee joint. You may feel something “pop” inside the knee. An initial inability to bear weight on the leg may subside and walking may be possible after several minutes. The knee may feel loose or that it is going to “give out” and return to sport is difficult. Over time, swelling will increase and motion may be lost.
What are the levels of severity in an ACL injury?
How is it diagnosed?
Dr Chandrasekaran will perform a thorough history and physical exam with X-rays. The physical examination will assess the extent of swelling, loss of motion, and strength.
Dr Chandrasekaran will perform maneuvers to check the stability of all the knee ligaments and the meniscus.
An MRI is helpful to confirm the diagnosis, showing the ACL tear. The type of tear (partial, complete, avulsion from either the tibia or femur) can be defined, which may assist in surgical planning. The MRI may also show bone bruising secondary to the injury.
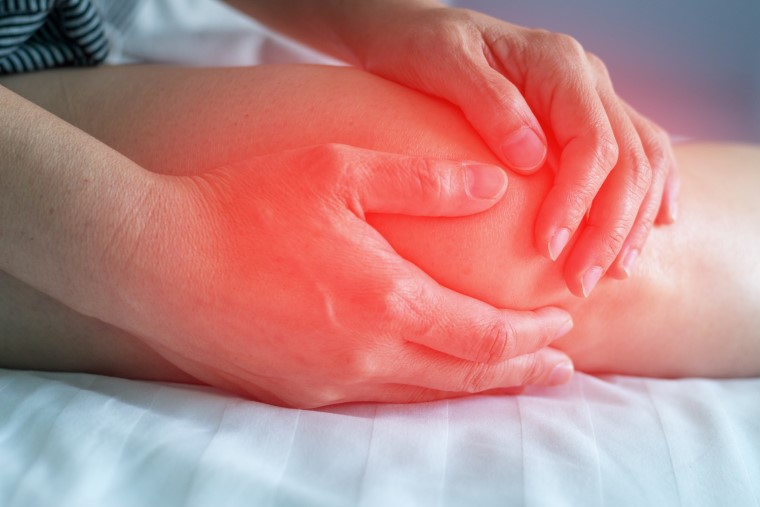
A “popping” sensation may be felt during the rupture of the ACL.
What is surgery recommended for an ACL injury?
How is an ACL rupture treated?
For the treatment of a rupture to the anterior cruciate ligament, ACL reconstruction is used. This surgery is considered gold-standard and is recommended to most when an ACL ruptures.
Pre-operative Measures
ACL tears do not heal. Some patients elect not to have reconstruction surgery. Non-operative treatment increases the risk of “wear and tear” arthritis and meniscus tears because of the instability in the joint.
Non-operative treatment consisting of anti-inflammatory medication, physical therapy, cryotherapy and activity modification may be prescribed prior to surgery to decrease the swelling, regain motion and strength, as research has demonstrated that surgery is less complicated and patients have better outcomes.
The ACL Reconstruction Surgery
Operative management of ACL tears varies depending on the type of tear experienced. ACL repair is accomplished through a minimally-invasive arthroscopic procedure during which your surgeon will place a small tube-like camera through an incision.
Two smaller incisions are placed around the treatment site to allow for the insertion of surgical tools. One smaller cut on the inside part of your leg is made to allow the extraction of the ACL graft (using either the hamstring tendons, patella, or quadriceps tendons) if autologous extraction is preferred in your case.
Using the images given by the camera, Dr Chandrasekaran will perform the arthroscopy. He will go on to replace the torn ACL with the graft and correct any further damage caused to the surrounding structures.
Once complete, your wound will be sutured. A drain may be left in place to prevent leakage of bodily fluids and to allow the wound to heal.
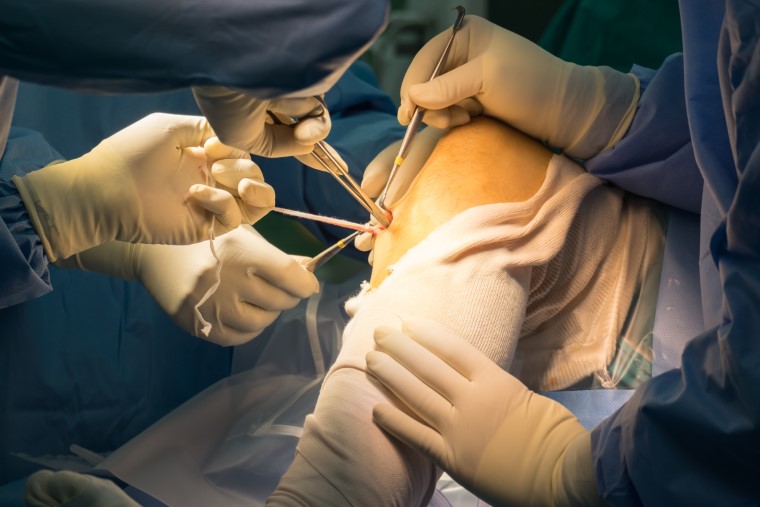
Surgery is performed arthroscopically, meaning that the procedure is minimally invasive and only a couple of small scars will be produced.
How long is the recovery after an ACL reconstruction?
The total recovery varies between individuals and depends on your pain tolerance, compliance with rehabilitation, and the desired activities that you wish to return to the following recovery. The recovery timeline for an ACL reconstruction is as follows:
Immediately after your procedure
Soreness and swelling are to be expected directly after your surgery. Dr Candrasekaran will prescribe pain medication to help you through the first couple of weeks. Your knee will be bandaged, and you will be expected to wear compression stockings to reduce your risk of developing deep vein thrombosis (DVT).
If you are seen as high risk for developing a DVT, you may be prescribed a course of blood-thinning medication for the duration of your immobility. You will remain in the hospital for observation until you are deemed fit for home, which is usually 1-2 days following surgery.
First Month
You will be given instruction to visit a physiotherapist who will provide you with exercises to help you regain mobility. You will still feel some pain and discomfort and be given crutches or a walking aid to help with getting around the house.
We recommend you continually rest your knee, keep it elevated, and use ice to reduce inflammation. Continue taking your anti-inflammatory medications for the time being, and wean off slowly as you feel your pain-reducing. Wound change may be necessary if the wound becomes oversaturated. Your doctor will reassess your wound for the presence of infection before replacing the bandage.
Months 2 - 3
Your first 2 to 4 weeks of the recovery focus heavily on regaining strength in your leg. You’ll be able to return to driving, walk on a treadmill, and perform light exercises given to you by your physiotherapist.
Month 2 onwards requires psychological strength as much as physical strength. You will begin to increase your confidence in your knee, understanding that its strength is similar to that of pre-surgery. This will be accomplished through continuous and strict adherence to physiotherapy.
Your bandage may also be removed around this time as your wound may have fully healed, depending on your body’s ability to heal.
Months 4 onwards
For some (athletes and younger people), full recovery may be seen at the 4-month mark. The aim at this point in recovery is to ensure that you can perform all your previous activities with no pain. Recovery may however take as long as 6 months depending on the individual. Our team will work with you until you feel comfortable performing your regular activities with confidence.

The aim of rehabilitation is to get you back to performing your regular activities, whether that may be a competitive sport or simply to go out for a brisk walk.
How much does an ACL reconstruction cost in Melbourne?
The total cost of an ACL reconstruction in our Melbourne clinic varies depending on the extent of your rupture and whether any further damage has been caused to the surrounding structures of the knee. Your total cost will incorporate the initial consultation fee of $200, alongside any additional follow-up appointments you may have ($100 each).
A breakdown of the total cost of your procedure will be given to you during your initial appointment with Dr Chandrasekaran.
Why choose MOATI and our doctor?
At MOATI, we thrive to provide you with exceptional levels of treatment and patient care with our years of experience and by focusing on the treatments we know work best. Our chief orthopaedic surgeon, Dr Siva Chandrasekaran, and his team take a patient-centred approach to treatment, ensuring each person is treated with the same level of high-quality care.

Our Melbourne orthopaedic surgeon, Dr Siva Chandrasekaran has completed three prestigious fellows from USA, Switzerland and the United Kingdom. Since then, he has gone on to publish over 50 articles about knee and hip treatments.
FAQs
Some of the most common questions surrounding ACL reconstruction surgery are answered below.
A rupture of the ACL can cause significant pain, lack of movement, inability to bear weight, and when left untreated, can cause arthritis.
Studies have shown that ACL reconstruction has success rates of 85-90%.
After your operation, you will be kept in hospital for one day for monitoring. You may be in pain, and so we will prescribe you a course of painkillers. Your wound will be bandaged, and you will be met by a physiotherapist who will help you learn the movements required to get out of bed and sit on a chair.
You will need crutches for at least the first 2 weeks of recovery.